Electrophysiology
Electrophysiology is the branch of cardiology that diagnoses and treats heart arrhythmias, or irregular heartbeats, caused by problems with the heart's electrical system. Arrhythmias can lead to uncomfortable symptoms and even put you at risk for developing more serious heart disease. At Cardiovascular Medicine, we are proud to have cardiac electrophysiologists who are specially trained and board certified in electrophysiology.
When to See a Cardiovascular Specialist
Heart arrhythmias can indicate or even result in more serious disease, so it’s important to visit a cardiac electrophysiologist if you have symptoms or risk factors. We provide a full spectrum of electrophysiology care, from diagnosis to treatment and management of your condition. We can help with:
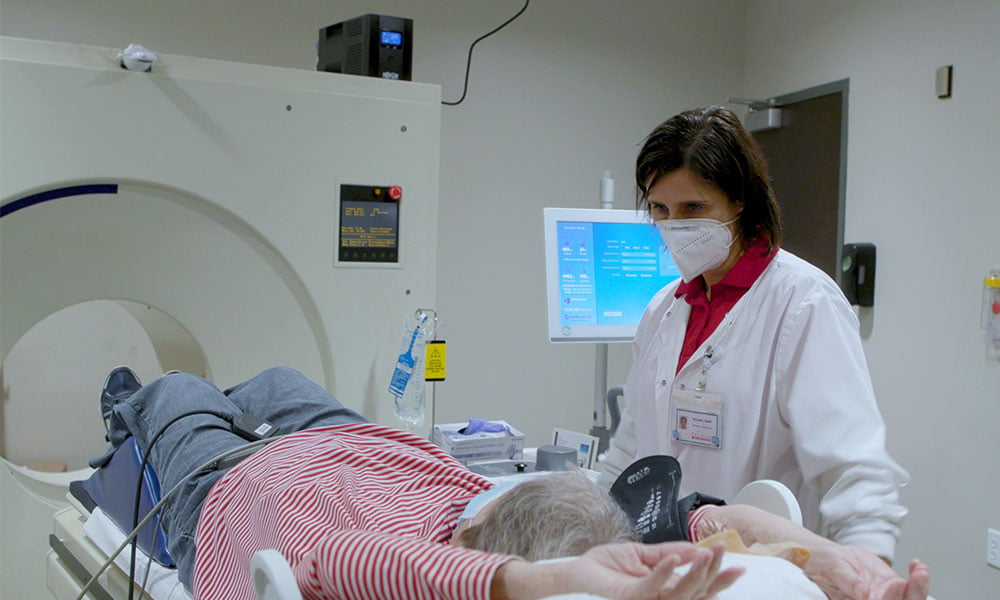
Diagnostic Testing
Understanding the cause of your arrhythmia is critical in deciding on the appropriate treatment. We offer many diagnostic tests that help us understand your heart’s functioning, including imaging so we can assess blood flow and monitoring so we can detect rhythm abnormalities. Our diagnostic testing options include:
Cardiovascular Treatments
Our mission is to provide personalized care to all patients. We create customized treatment plans based on your testing results, personal history, preferences, and more. With Cardiovascular Medicine, you can rest assured that you are getting the most advanced cardiovascular care in the Quad Cities area. Your options for treatment may include:
Pacemaker and Defibrillator Insertions & Monitoring
Pacemakers vs. Defibrillators
Your heart's electrical system is in control of maintaining a normal, steady rhythm. Heart disease can interfere with the heart's proper functioning, which can cause damage or even cardiac arrest. Pacemakers and defibrillators are implantable devices that help maintain proper heart functioning. Though both ensure your heart keeps a normal rhythm, they differ slightly in their purposes and how they work. At Cardiovascular Medicine, we have experienced cardiac electrophysiologists who help determine the best choice for your situation.
What to Expect During Insertion
Pacemaker Insertion
Implanting a pacemaker typically takes a few hours. Before the procedure, we will administer an IV with a sedative so you can relax. We use conscious sedation for most pacemaker insertions; however, in certain cases, we may need to use general anesthesia, where you will be fully asleep.
Using a major vein near your collarbone, we will insert one or more wires and guide them to your heart with the help of X-ray images. For each wire, one end is inserted in the necessary area of your heart, while the other end attaches to the pulse generator, which we usually place beneath your collarbone.
A leadless pacemaker is smaller, with the pulse generator and leads contained in a single capsule. As such, this surgery is less invasive. We will use a vein in the groin to guide the pacemaker to the right position near the heart.
Implantable Cardioverter Defibrillator (ICD)
Implantation of an ICD will take a few hours. The most common procedure is the transvenous approach, which involves a small incision at your collarbone.
We’ll begin with an IV and sedative. We will make an incision near the collarbone or, in some cases, your chest or abdomen. Gaining access through your vein, we put the wires into the heart chambers. The ICD goes in a pouch under the skin. We ensure the leads are connected to both the heart and ICD and that they work properly. Before we end the procedure, we test the device to make sure everything is working as it should.
Recovery
For both a pacemaker and ICD implantation, you will likely go home from the hospital the day after the procedure. You will need to have someone drive you home. You may feel tired and sore at the site of the incision. Your doctor will advise you on the best medication to take for any pain.
Before you go home, we will program the pacemaker to suit your heart rhythm needs. Your doctor will discuss any precautions you need to take around things like cell phones or certain medical equipment.
We may test the ICD system once again before you leave.
In general, you should refrain from heavy lifting and vigorous activity in the month after the procedure. Avoid putting pressure on the implantation site.
To help you manage your device, we offer device clinics at our Davenport and Moline Offices. Our dedicated clinical staff is specially trained in electrophysiology and in the care of implanted devices. They are here to help you with any follow-up care you need for your pacemaker or ICD.
Risks & Side Effects
Both pacemaker and ICD implantations are generally safe, and complications are uncommon.
Am I a Candidate?
A pacemaker is most often recommended for people who have bradycardia, when the heart beats too slowly. In some cases, it may be used for people whose heart beats too fast (tachycardia) or to correct an arrhythmia.
ICDs are for people who have certain heart conditions that cannot be managed with other treatments. They guard against sudden cardiac death from life-threatening abnormal heart rhythms.
More on Pacemakers and Defibrillator Insertions
What is the Difference Between a Pacemaker and a Defibrillator?
Pacemakers
Pacemakers are used to prevent the heart from beating too slowly when you have a chronic slow or irregular heartbeat. They can also help treat heart failure by ensuring normal heart function. Pacemakers work consistently to maintain a normal heart rate. They send electrical signals to your heart when they detect a slow or irregular heartbeat.
A pacemaker has two parts: a pulse generator and leads. The pulse generator controls when electrical pulses are sent to the heart, and the leads (electrodes), which are attached to chambers of your heart, deliver the electric signals to restore a normal heart rate.
Defibrillators
Defibrillators are similar to pacemakers in that they work to ensure your heart maintains a safe and normal rhythm. The difference lies in the defibrillator's ability to send an electrical shock to the heart when it detects a fatal rhythm.
An implantable cardioverter defibrillator (ICD) monitors your heart and sends an electric shock to stabilize your heart rate when needed. The battery-controlled device works to correct life-threatening arrhythmia to prevent cardiac arrest.
Situated under your skin, an ICD monitors your heart rate and sends electrical shocks to correct the heart rhythm when needed. It is the size of a stopwatch with leads that go directly into your heart chambers. These leads are what deliver the electrical signals.
Some ICDs also function as pacemakers.
Uncommon Complications and Risks of Pacemaker and ICD Implantations
- Bleeding, bruising, or swelling
- Collapsed lung (pneumothorax)
- Damage to blood vessels or nerves from the leads
- Infection of the incision site
- Movement of the device, which can damage internal tissue
- Blood clots near device site
- Blood in the space between the lung and chest wall (hemothorax)
Who Are Pacemakers Recommended For?
We may recommend pacemakers for those who have or have had:
- Heart attack
- Heart failure
- An enlarged heart muscle
- Congenital heart defects
Who is Considered In Need of an ICD?
Reasons we may consider you high-risk and in need of an ICD include:
- Experiencing abnormal heart rhythms such as ventricular tachycardia or ventricular fibrillation
- Previous heart attacks
- Heart failure
- Cardiomyopathy
- Congenital heart defect
Meet Your Illinois and Iowa
Cardiovascular Physicians
CVM Locations
Insurance Providers We Accept
In Search of Care? Request a Consultation Today



