Procedural Lab
At Cardiovascular Medicine, we want to make care as convenient as possible. To this end, we offer several in-office peripheral vascular services in our state-of-the-art procedural lab. Our lab features one of the most technologically advanced vascular imaging systems available in an office setting. Using high-tech equipment, our experienced cardiovascular physician specialists can detect and treat peripheral vascular disease on an outpatient basis.
When to See an Interventional Cardiologist
Peripheral vascular conditions occur when your peripheral arteries are narrowed or blocked, resulting in a lack of adequate blood flow. This can lead to painful symptoms, as well as put you at risk for serious complications such as amputation or stroke. Therefore, if you are at risk for peripheral arterial disease or are experiencing possible symptoms, it’s important to make an appointment to explore what’s going on. We can assess:
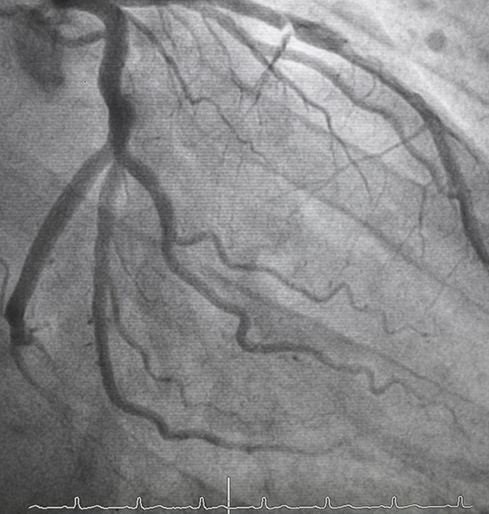
Diagnostic Testing
To examine your peripheral arteries, we use angiography, an imaging technique that uses X-ray and contrast dye to see how efficiently blood is flowing. The contrast dye provides improved visualization so we can identify areas of narrowing or blockage. We use minimally-invasive procedures to detect abnormalities in your extremities and kidneys, including:
Peripheral Vascular Treatments
We are proud to offer peripheral vascular services in-office to treat your narrowed or blocked peripheral arteries. By providing these services in our office, our patients experience the convenience of a safe, accessible environment, along with a predictable schedule and a lower cost. Our procedures are minimally-invasive and allow you to return to your normal activities sooner. Discover more about our procedural lab treatments.
Peripheral Vascular Intervention Procedures
What is Peripheral Vascular Intervention?
Narrowed or blocked arteries in your arms, legs, and trunk result in reduced blood flow, interfering with healthy circulation, is known as peripheral vascular intervention. Often caused by peripheral vascular disease, this condition can cause issues such as leg pain, kidney problems, high blood pressure, or even stroke. Alleviating these symptoms involves opening the blocked peripheral arteries with treatments known as peripheral vascular intervention procedures.
We offer two minimally-invasive peripheral vascular intervention procedures: peripheral angioplasty and peripheral atherectomy. These procedures are performed in our office, and they can be done independently or in combination.
Peripheral vascular interventions help open up your arteries to improve blood flow. We recommend the procedures for those who have narrowed or blocked arteries from plaque buildup inside the artery walls.
When plaque, composed of fatty deposits, accumulates in blood vessels, it is a condition known as atherosclerosis. Left untreated, atherosclerosis can lead to serious complications. Having peripheral vascular intervention procedures can help prevent the condition from progressing and help you feel better again.
Vascular Treatments
Peripheral Angioplasty
Peripheral angioplasty uses a tiny balloon catheter to widen blood vessels and improve blood flow for the peripheral parts of the body, such as the legs, arms, or renal arteries. It is sometimes used in conjunction with a stent, a small wire mesh tube that helps prop the artery open to prevent it from narrowing again.
We are able to perform this minimally-invasive procedure in our office. It will take several hours, depending on how many blockages you have.
Peripheral Atherectomy
Peripheral atherectomy is designed to cut through plaque and calcium buildup in the blood vessels. It is performed using a catheter with a sharp blade, which reduces the plaque to tiny particles, smaller than red blood cells. The inner surface of the vessel is left smoother and more open, allowing blood to flow more freely through the vessel. Sometimes, a laser is used to open the artery, which vaporizes the plaque and smoothing the vessel lining.
Peripheral atherectomy takes about two hours, though preparation and recovery will add to the total time. We are able to perform the procedure in our office.
Recovery
Both peripheral angioplasty and peripheral atherectomy are minimally-invasive procedures, so your recovery should not be extensive. We will ask you to rest in our recovery room for a few hours so we can observe you post-procedure. You will need to lay still for a few hours to allow the site of the catheter insertion to heal. Drink plenty of water to flush any contrast dye from your system.
You should be able to resume most normal activity about a week after your procedure. Both procedures are designed to provide significant relief from your symptoms. Our goal is to:
- Ease your pain and discomfort
- Manage your atherosclerosis
- Reduce your risk of serious complications
Risks & Side Effects
Peripheral vascular interventions use X-ray and contrast dye to help us see inside your blood vessels. X-ray use comes with a small amount of radiation exposure. Please talk to us about any concerns you have with X-ray. We don’t recommend the procedures if you’re pregnant. Some of the risks associated with an atherectomy include:
- Embolism
- Re-blockage of an artery
- Allergy to the dye
- Impaired kidney function
Am I a Candidate?
If you have been diagnosed with atherosclerosis or peripheral arterial disease, a peripheral angioplasty or atherectomy could alleviate your symptoms, which may include:
- Leg discomfort, pain, or cramping with activity
- Leg numbness or weakness
- Heavy feet/legs
- Erectile dysfunction
- Slow toenail or leg hair growth
- Burning or aching in your toes while resting
- Cold legs or feet
- Wounds and sores that won’t heal
More on Peripheral Vascular Interventions
Uncommon Complications
Though rare, complications that could arise from angioplasty include:
- Bleeding
- Blood clots
- Re-narrowing of the artery
- Kidney failure from the contrast dye
- Allergic reaction to the contrast dye
- Breathing problems
- Infection
- Rupture of your artery
What is an Embolism?
Factors That Increase Your Risk of Developing Peripheral Arterial Disease
Your risk of developing peripheral arterial disease depends on several factors. These include:
- Smoking
- High cholesterol
- High blood pressure
- Obesity
- Older age
- Being male
- Family history of heart or blood vessel disease
Meet Your Illinois and Iowa
Cardiovascular Physicians
CVM Locations
Insurance Providers We Accept
In Search of Care? Request a Consultation Today



